ResveratrolConsumer
avert online
consumer fraud
ResveratrolQuiz
test your knowledge
New E-Book
How the world got lost on
the road to an anti-aging pill
Subscribe to our newsletter to receive email notifications when new articles are posted.
September 30, 2012: by Bill Sardi
Modern medicine becomes more and more disingenuous every day. Expensive cures preferred over more effective and less problematic natural remedies. An example of this is presented below. A report published at Science Daily shows that white blood cells called macrophages accumulate cholesterol in their attempt to remove excesses from the circulatory system. However, cholesterol over-bloated macrophages will become what are called foam cells that then trigger inflammation within arteries. So researchers claim they have altered an old problematic drug to facilitate exit (efflux) of cholesterol from macrophages. It’s heralded as a breakthrough. But they ignore the fact that resveratrol, a natural molecule, does the same thing. See the report below published in 2006 showing resveratrol limits cholesterol accumulation in human macrophages. By the way, the researchers are conceding their long-held idea of lowering cholesterol production in the liver has been a misdirection. — Copyright 2012 Resveratrolnews.com
http://www.sciencedaily.com/releases/2012/09/120927123640.htm
ScienceDaily (Sep. 27, 2012) — Atherosclerosis — the hardening of arteries that is a primary cause of cardiovascular disease and death — has long been presumed to be the fateful consequence of complicated interactions between overabundant cholesterol and resulting inflammation in the heart and blood vessels.
However, researchers at the University of California, San Diego School of Medicine, with colleagues at institutions across the country, say the relationship is not exactly what it appears, and that a precursor to cholesterol actually suppresses inflammatory response genes. This precursor molecule could provide a new target for drugs designed to treat atherosclerosis, which kills tens of thousands of Americans annually.
The findings are published in the September 28, 2012 issue of Cell.
Lurking within our arterial walls are immune system cells called macrophages (Greek for “big eater”) whose essential function is to consume other cells or matter identified as foreign or dangerous. “When they do that, it means they consume the other cell’s store of cholesterol,” said Christopher Glass, MD, PhD, a professor in the Departments of Medicine and Cellular and Molecular Medicine and senior author of the Cell study. “As a result, they’ve developed very effective ways to metabolize the excess cholesterol and get rid of it.”
But some macrophages fail to properly dispose of the excess cholesterol, allowing it to instead accumulate inside them as foamy lipid (fat) droplets, which gives the cells their particular name: macrophage foam cells.
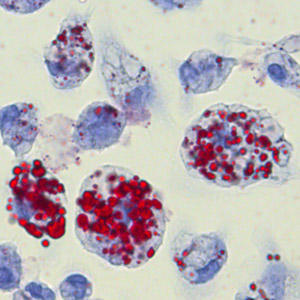
When macrophages take up massive amounts of cholesterol they form “foam cells,” characterized by multiple lipid droplets (stained red). (Credit: Image courtesy of Marten Hoeksema, University of Amsterdam.)
These foam macrophages produce molecules that summon other immune cells and release molecules, signaling certain genes to launch an inflammatory response. Glass said conventional wisdom has long assumed atherosclerotic lesions — clumps of fat-laden foam cells massed within arterial walls — were the unhealthy consequence of an escalating association between unregulated cholesterol accumulation and inflammation.
Glass and colleagues wanted to know exactly how cholesterol accumulation led to inflammation, and why the macrophages failed to do their job. Using specialized mouse models that produced abundant macrophage foam cells, they made two unexpected discoveries that upend previous assumptions about how lesions form and how atherosclerosis might be more effectively treated.
“The first is that foam cell formation suppressed activation of genes that promote inflammation. That’s exactly the opposite of what we thought happened,” said Glass. “Second, we identified a molecule that helps normal macrophages manage cholesterol balance. When it’s in abundance, it turns on cellular pathways to get rid of cholesterol and turns off pathways for producing more cholesterol.”
That molecule is desmosterol — the final precursor in the production of cholesterol, which cells make and use as a structural component of their membranes. In atherosclerotic lesions, Glass said the normal function of desmosterol appears to be “crippled.”
“That’s the next thing to study; why that happens,” Glass said, hypothesizing that the cause may be linked to overwhelming, pro-inflammatory signals coming from proteins called Toll-like receptors on macrophages and other cells that, like macrophages, are critical elements of the immune system.
The identification of desmosterol’s ability to reduce macrophage cholesterol presents researchers and drug developers with a potential new target for reducing the risk of atherosclerosis.
Glass noted that a synthetic molecule similar to desmosterol already exists, offering an immediate test-case for new studies. In addition, scientists in the 1950s developed a drug called triparanol that inhibited cholesterol production, effectively boosting desmosterol levels. The drug was sold as a heart disease medication, but later discovered to cause severe side effects, including blindness from an unusual form of cataracts. It was pulled from the market and abandoned.
“We’ve learned a lot in 50 years,” said Glass. “Maybe there’s a way now to create a new drug that mimics the cholesterol inhibition without the side effects.”
Co-authors are first author Nathanael J. Spann, Norihito Shibata, Donna Reichart, Jesse N. Fox and Daniel Heudobler, UCSD Department of Cellular and Molecular Medicine; Lana X. Garmire, UCSD Department of Bioengineering; Jeffrey G. McDonald and David W. Russell, Department of Molecular Genetics, UT Southwestern Medical Center; David S. Myers, Stephen B. Milne and Alex Brown, Department of Pharmacology, Vanderbilt Institute of Chemical Biology; Iftach Shaked and Klaus Ley, La Jolla Institute of Allergy and Immunology; Christian R.H. Raetz, Department of Biochemistry, Duke University School of Medicine; Elaine W. Wang, Samuel L. Kelly, M. Cameron Sullards and Alfred H. Merrill, Jr., Schools of Biology, Chemistry and Biochemistry and the Parker H. Petit Institute of Bioengineering and Bioscience, George Institute of Technology; Edward A. Dennis, UCSD Department of Chemistry and Biochemistry; Andrew C. Li, Sotirios Tsimikas and Oswald Quehenberger, UCSD Department of Medicine; Eoin Fahy, UCSD Department of Bioengineering; and Shankar Subramaniam, UCSD Departments of Cellular and Molecular Medicine, Bioengineering and Chemistry and Biochemistry.
Funding for this research came, in part, from National Institutes of Health grants GM U54069338 (to the LIPID MAPS Consortium), P01 HC088093 and P01 DK074868.
Journal Reference:
Nathanael J. Spann, Lana X. Garmire, Jeffrey G. McDonald, David S. Myers, Stephen B. Milne, Norihito Shibata, Donna Reichart, Jesse N. Fox, Iftach Shaked, Daniel Heudobler, Christian R.H. Raetz, Elaine W. Wang, Samuel L. Kelly, M. Cameron Sullards, Robert C. Murphy, Alfred H. Merrill, H. Alex Brown, Edward A. Dennis, Andrew C. Li, Klaus Ley, Sotirios Tsimikas, Eoin Fahy, Shankar Subramaniam, Oswald Quehenberger, David W. Russell, Christopher K. Glass. Regulated Accumulation of Desmosterol Integrates Macrophage Lipid Metabolism and Inflammatory Responses. Cell, 2012; 151 (1): 138 DOI: 10.1016/j.cell.2012.06.054
Biochem Biophys Res Commun. 2006 Sep 29;348(3):1047-54. Epub 2006 Aug 1.
Sevov M, Elfineh L, Cavelier LB.
Department of Genetics and Pathology, Rudbeck Laboratory, Uppsala University, Sweden.
The naturally occurring polyphenol resveratrol has been associated with the beneficial effects of red wine consumption on cardiovascular disease and shown to inhibit atherosclerosis in animal models. To determine if resveratrol affects the expression of genes that control lipid homeostasis in human macrophages, we measured expression changes in the LXR-alpha pathway, crucial to cholesterol efflux (exit), and in genes that mediate lipoprotein uptake. Resveratrol treatment of THP-1 macrophages induced LXR-alpha at mRNA and protein levels. Increased recruitment of RNA polymerase II to the LXR-alpha promoter suggested that up-regulation was at least partly mediated by transcriptional mechanisms. Resveratrol also induced LXR-alpha in human monocyte-derived macrophages together with elevated ABCA1 and ABCG1 mRNA levels. Moreover, resveratrolrepressed the expression of the lipid uptake genes LPL and SR-AII. The ability of resveratrol to modulate expression of the genes involved in lipid uptake and efflux suggests that polyphenols can potentially limit cholesterol accumulation in human macrophages.
PMID: 16901463
Posted in Resveratrol
Add comments »